
Pregnancy and Birth
Latest News
Latest Videos

Shorts









Podcasts
CME Content
More News

The AAP'S 2026 schedule has been endorsed by 12 medical and health organizations, including the American College of Nurse Midwives and the American College of Obstetricians and Gynecologists.

In patients with diet-controlled gestational diabetes, continuing pregnancy beyond 39 weeks was associated with increasing maternal and neonatal risks.

A large cohort study found that prenatal exposure to acid-suppressive medications was not associated with neuropsychiatric disorders in children.

A nationwide Norwegian cohort study suggests that prenatal factors, including fetal growth and maternal diabetes, may influence the risk of developing multiple sclerosis in adulthood.

A phase 3 trial of oral brexanolone for postpartum depression will continue unchanged following a favorable DSMB safety review.

A population-based study links minimum wage increases to improved maternal cardiovascular health during pregnancy.

A large California cohort study shows that aggregating Asian American and Pacific Islander populations can obscure substantial differences in hypertensive disorder risk during pregnancy.

Analysis of internal FDA records reveals that mifepristone’s REMS program was shaped by repeated evidence-based safety reviews.

Maternal influenza and Tdap vaccination during pregnancy was associated with fewer influenza- and pertussis-related hospital and ED visits in infants younger than 6 months.

Screen-guided care using the PreTRM blood test reduced preterm birth–related complications and NICU use.

New research links abnormal collagen remodeling at cesarean scars—not placental invasion—to placenta accreta spectrum risk.
A study links opioid-related diagnoses during pregnancy to increased maternal morbidity and neonatal complications.

A randomized trial found that real-time continuous glucose monitoring reduced large-for-gestational-age births compared with self-monitoring in gestational diabetes.

Higher maternal vitamin D levels in pregnancy were associated with reduced odds of early childhood caries and lower DMFT scores in offspring.

A new study reveals 3 NAD-related metabolites elevated in women with recurrent miscarriage, indicating potential risk identification.

Discontinuing GLP-1 receptor agonists before or early in pregnancy was associated with greater gestational weight gain and higher risks of diabetes, hypertension, and preterm birth.

New data highlight how optical genome mapping can uncover chromosomal abnormalities missed by traditional tests.

A review reported insufficient evidence connecting prenatal paracetamol exposure to autism or ADHD.

Holiday meals carry extra food safety risks for pregnant patients. Here’s what ob-gyns should remind them before Thanksgiving gatherings.

Planned community births in Oregon showed increased risks only when hospital transfer occurred, underscoring the need for clear counseling and transfer systems.

Two-thirds of pregnancies fall outside recommended gestational weight gain ranges, increasing risks for adverse maternal and neonatal outcomes.
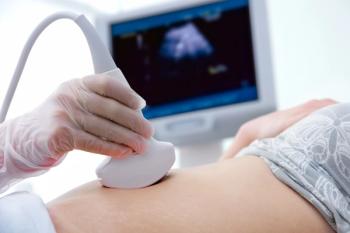
Obstetric ultrasound of pregnancies less than 10 weeks gestational duration is an essential skill for the obstetric provider and has unique considerations.

A review found no causal link between prenatal acetaminophen exposure and offspring neurodevelopmental disorders.

Survey reveals limited allergy referrals in pregnancy due to lack of guidance and long wait times, highlighting need for better education.

The FDA updates acetaminophen warnings for pregnant women and approves leucovorin for treating cerebral folate deficiency.



















