Association of higher dairy intake with BMD
A recent study examined why Puerto Rican adults have a high prevalence of osteoporosis and vitamin D deficiency and what role dairy intake has on BMD.
Although dairy foods improve bone mineral density (BMD) in non-Hispanic whites, little is known about whether there is a similar connection in Puerto Rican adults.
To better understand why that population has a high prevalence of osteoporosis and vitamin D deficiency, a recent
The study found that dairy food intakes were linked to higher BMD, especially among adults with sufficient vitamin D status.
Data from 904 participants of BPROS, all of whom were Puerto Rican adults living in the Greater Boston area, were analyzed. Overall, 73% of the sample were women, of whom 87% were postmenopausal. The mean age of the sample was 60.0 years, with a mean body mass index (BMI) of 32.3 kg/m2.
The analysis was based on dietary intakes with a culturally tailored food-frequency questionnaire. Dairy food groups were calculated: total dairy, modified dairy (without cream or dairy desserts), fluid dairy (milk + yogurt), cheese, yogurt, and cream and desserts.
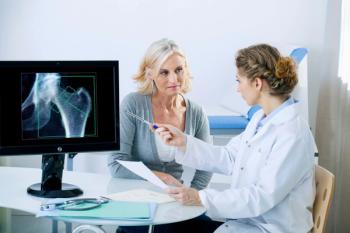
BMD (g/cm2) was measured using dual-energy X-ray absorptiometry. Vitamin D status was defined as either sufficient (serum 25-hydroxyvitamin D [25(OH)D] ≥ 20 ng/mL) or insufficient (< 20 ng/mL).
Mean serum 25(OH)D was 14.3 ng/mL among individuals with sufficient vitamin D levels versus 26.0 ng/mL in those whose levels were insufficient.
Higher intake of modified dairy foods (β = 0.0015, P = 0.02) and milk (β = 0.0018, P = 0.04) was linked to higher femoral neck (FN) BMD.
In addition, participants who were vitamin D-sufficient, had higher intake of total dairy (P = 0.03 to 0.07), fluid dairy (P = 0.01 to 0.05) and milk (P = 0.02 to 0.09) were much more likely to have higher FN and lumbar spine BMD.
Conversely, for those who were vitamin D-insufficient, dairy intake was not associated with BMD (P range = 0.11 to 0.94).
In summary, the study cohort had a relatively low total diary intake of roughly 1.5 servings per day, excluding cream and dessert dairy products. This is far lower than the current recommendation of three servings of dairy foods daily.
The highest percentage of dairy food intake from individual sources was from fluid dairy, consisting of a composite variable of milk and yogurt and representing about 7.1% of total energy intake. Full-fat dairy contributed approximately 8.7% of energy intake, whereas reduced-fat dairy represented 4.1%.
The average total (food + supplement) calcium intake of 1005 mg/d and vitamin D intake of 6.9 μg/d were also below national recommendations for this age group: 1200 mg/d and 15 to 20 μg/d, respectively.
One drawback of the current study is reliance on self-reported dietary information. Nonetheless, the authors expect the rate of osteoporosis-related fractures to continue to increase by 175% in Puerto Rican men and women. “It is vital to determine whether dairy intake influences bone health among this growing US subgroup,” they wrote.
Besides considering culturally acceptable dairy food sources, future intervention studies should account for improvements in lifestyle behaviors known to affect bone, according to the authors, including increased physical activity and elevated intake of fruit, vegetables and fiber, while reducing intake of refined grains and saturated and omega-6 fats.