Changes in bone density linked to reduced fracture risk
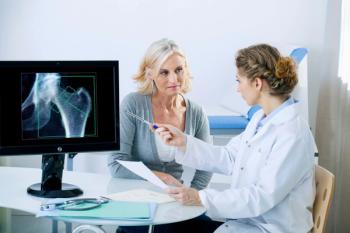
A meta-regression of published trials has concluded that larger improvements in bone mineral density (BMD) via dual‐energy X‐ray absorptiometry (DXA) are associated with greater reductions in fracture risk.
Building on prior observations, a
“Although these results cannot be directly applied to predict the treatment benefit in an individual patient, they provide compelling evidence that improvements in BMD with osteoporosis therapies may be useful surrogate endpoints for fracture in trials of new therapeutic agents,” the authors wrote.
Methods
The investigators selected 38 placeboâcontrolled studies involving 19 therapeutic agents to determine the connection between improvements in BMD and reductions in fracture risk. The studies evaluated six bisphosphonates (20 trials); four selective estrogen receptors modulators (SERMS) (5 trials); calcitonin/estrogen compounds (2 trials); tibolone (1 trial); an anti-Rank Ligand antibody (2 trials); parathyroid hormone (PTH) (1-84) (1 trial); two PTH analogs (4 trials), an anti-sclerostin antibody (1 trial) and a cathepsin K inhibitor (1 trial).
Individual trial sizes ranged from 246 to more than 16,000 participants, with 1 to 8 years of follow-up. Of the 38 studies, 32 were limited to postmenopausal women, whereas 5 trials enrolled both men and women and one trial men only.
Results
Greater improvements in BMD were strongly linked to greater reductions in vertebral and hip fractures, but not nonvertebral fractures.
For vertebral fracture, the R-squared (r2) values for total hip, femoral neck and lumbar spine BMD change were 0.56, 0.54, and 0.63, respectively (P ≤ 0.0002). Estimates of reduction in fracture risks were based on roughly the lowest difference and the highest difference in BMD, which were 2% and 6% for the hip and 2% and 14% for the lumbar spine, respectively.
A 2% improvement in total hip BMD resulted in a 28% reduction in vertebral fracture, compared to a 66% reduction with a 6% improvement in total hip BMD. Similarly, a 2% improvement in lumbar spine BMD achieved a 28% reduction in vertebral fracture. Furthermore, 8% and 14% improvements in lumbar spine BMD resulted in 62% and 79% reductions in vertebral fractures, respectively.
The analysis also found that for hip fracture, the r2values for total hip, femoral neck, and lumbar spine BMD change were 0.48 (P= 0.01), 0.42 (P = 0.02) and 0.22 (not significant), respectively. For instance, a 2% improvement in total hip BMD achieved a 16% reduction in hip fracture, while a 6% improvement in total hip BMD attained a 40% reduction in hip fracture. These results were similar for femoral neck BMD. Conversely, there was a weaker association between improvements in lumbar spine BMD and hip fracture, which did not reach statistical significance.
Limitations
A major study limitation is that because data were pooled from trials that lasted from 1 to 8 years, the varying time durations impacted at least some outcomes. “For example, bisphosphonates strongly increase BMD over the first year of treatment with smaller decreases over the next 2 to 3 years and then a plateau,” noted the authors. Likewise, fracture reductions normally do not manifest until after 18 to 24 months of treatment.
Newsletter
Get the latest clinical updates, case studies, and expert commentary in obstetric and gynecologic care. Sign up now to stay informed.