Up to 1% of patients may experience myeldysplastic syndrome or acute alceloid leukemia, which have been associated with several PARPi.
PARP inhibitors: Choosing what to use in epithelial ovarian cancer
Across different drugs and clinical settings, use of PARPi has resulted in a prolonged period without cancer recurrence.
Since the discovery of PARP inhibitors (PARPi) in 2005, there has been rapid clinical development of five different agents (olaparib, rucaparib, niraparib, veliparib, talazoparib), leading to seven indications approved by the US Food and Drug Administration (FDA) across breast and ovarian cancer.
In 2014, olaparib became the first PARPi approved by the FDA for use as treatment of recurrent ovarian cancer, followed by rucaparib in 2016 and niraparib in 2019.
Over this same time period, the FDA approved all three of these PARPi for a different indication – as maintenance therapy intended to prolong the disease-free interval following chemotherapy.
Across different drugs and clinical settings, use of PARPi has resulted in a prolonged period without cancer recurrence – or disease-free interval – particularly among patients with BRCA1 and BRCA2 mutations, owing to their mechanism of action.
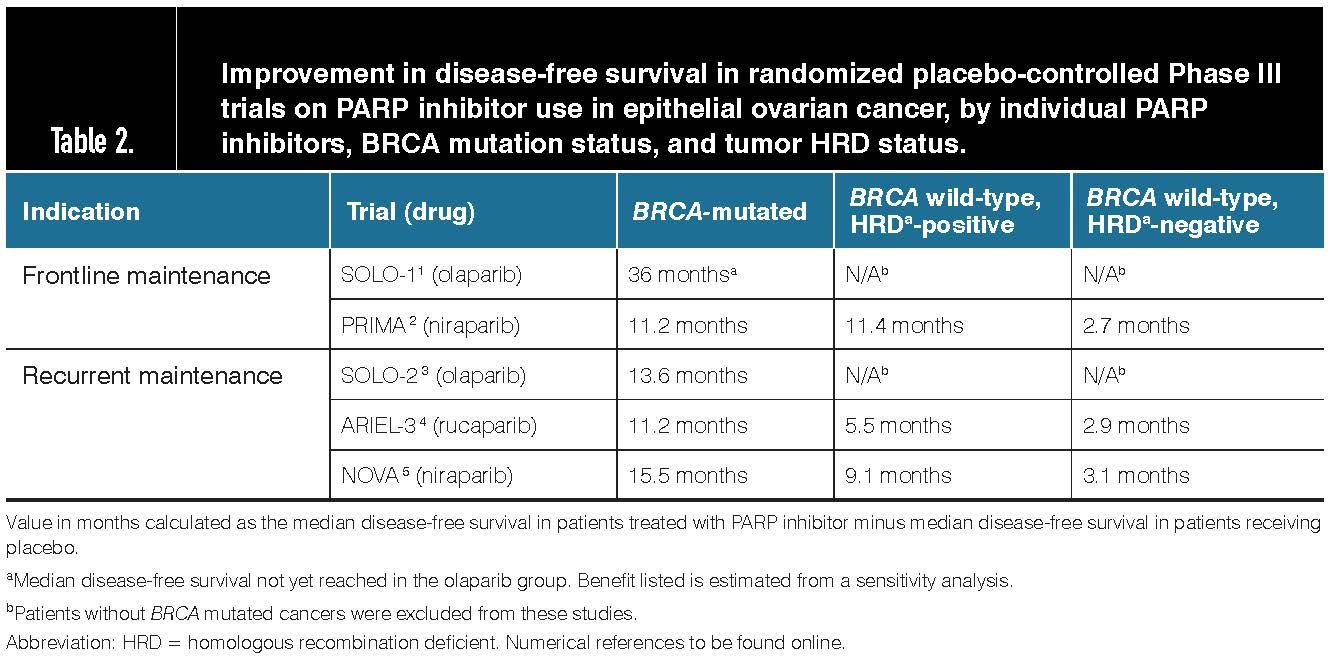
Improvement in disease-free survival in randomized placebo-controlled Phase III trials on PARP inhibitor use in epithelial ovarian cancer, by individual PARP inhibitors, BRCA mutation status, and tumor HRD status.

PARPi are a class of oral targeted therapy whose effect is dependent upon a tumor’s inability to repair its DNA. The PARP1 and PARP2 proteins are instrumental in repairing DNA single-strand breaks, which prevents formation of double-strand breaks at the time of DNA replication.
PARPi block this repair process and thus dramatically increase the number of double strand breaks. Cells can typically repair these resultant double strand breaks in an error-free fashion using the homologous recombination (HR) pathway, but when the pathway is defective, PARPi result in cell death.
This homologous recombination deficiency (HRD) is frequently a result of a germline or somatic mutation in a gene involved in the HR pathway, notably BRCA1 and BRCA2, but can also be detected in tumors in the absence of such mutations.
With germline and somatic testing, patients with genetic mutations or tumors with HRD can be identified as those who may derive significant clinical benefit from PARPi use.
With more than 20 trials of PARPi in ovarian cancer alone, there is a growing body of literature on the common side effects of these drugs and their management, as well as their unique financial challenges.
Ongoing clinical questions being addressed include how best to predict patient response to PARPi therapy, combat drug resistance, and determine the optimal setting(s) for use in individual patients.
Adverse effects with PARPi use
GENERAL
Many of the adverse events (AEs) encountered with use of PARPi are shared across agents. Most patients experience some degree of nausea and fatigue. Serious hematologic side effects can occur with any PARPi, and myelosuppressive effects can be exacerbated when these drugs are combined with other therapies.
Dose reductions are often necessary in the event of a serious side effect, and if they persist, the drug may need to be discontinued. Of note, myelodysplastic syndrome (MDS) and acute myeloid leukemia (AML) are serious but rare AEs occurring in up to 1% of patients and they have been associated with several different PARPi.
Embryo-fetal toxicity has been documented in animal studies with exposure to PARPi. These drugs should not be used in pregnant patients, and pregnancy should be avoided for 6 months following last exposure.1-4
INDIVIDUAL PARPI SIDE EFFECTS
Olaparib was the first PARPi to be developed thus is the most extensively studied. The most common AEs with olaparib are fatigue, nausea, and vomiting, which occur in 60% to 75% of patients across studies.
Serious hematologic AEs can occur in 10% to 20% of patients (anemia, neutropenia), and rarely patients experience severe fatigue (4%).5,6 Olaparib in combination with vascular endothelial growth factor (VEGF) inhibitors such as bevacizumab or cediranib can increase the rate of hypertension, fatigue, diarrhea, abdominal pain, and small bowel obstruction.7
The AE profile of rucaparib is similar to that of olaparib, with nausea and fatigue occurring in more than 70% of patients, and severe anemia in about one-fifth of patients.
An isolated transaminitis is a unique AE with rucaparib use, resulting in mild to moderate elevations of alanine transaminase (ALT) and aspartate transaminase (AST) noted in one-third of patients and more serious elevations in approximately 10% of patients. Rash and photosensitivity were other specific yet uncommon mild AEs.8,9
Myelosuppression is more frequent among patients taking niraparib, with significantly more thrombocytopenia in particular compared to other PARPi (up to 60% of patients). Notable serious AEs with niraparib are also hematologic, with significant anemia being the most common (25%-30%), followed by thrombocytopenia (20%-30%) and neutropenia (10%-20%).
Mild nausea and fatigue are seen at rates similar to those in olaparib and rucaparib, and mild constipation can be encountered as well.10
Although not FDA-approved for use in the United States, veliparib has shown some efficacy as both monotherapy and in combination with other cancer-directed treatments in numerous trials. Gastrointestinal (GI) AEs were similar to other PARPi, and severe AEs were relatively uncommon.11
Talazoparib is only FDA-approved for treatment in patients with advanced breast cancer who have germline BRCA mutations (Table 1). Although fatigue and GI AEs are milder with talazoparib relative to other PARPi, severe hematologic AEs occur in up to 55% of patients.12
MONITORING
All PARPi require close monitoring with weekly complete blood count with differential for the first month of therapy, which can be done once a month thereafter, if the patient is stable. A complete metabolic panel should be obtained at baseline and periodically thereafter.
Cholesterol should be monitored with rucaparib use. Niraparib may result in hypertension, so close observation of blood pressure at baseline and during the first month of therapy is advised.
MANAGING AES
Although patients may already experience some of the symptoms discussed above at baseline due to prior therapies or disease burden, adequate management of symptoms after starting a PARPi is critical, as these AEs can have a significant impact on physical and psychological well-being.
Anticipatory counseling about the likelihood of certain symptoms can reduce early discontinuation of drugs due to discomfort from AEs. Given the frequency of nausea, it is important to encourage use of antiemetics and counsel patients that these symptoms can abate after the first 1 to 2 months.
Common interventions such as exercise and caffeine can be encouraged to improve fatigue, and over-the-counter pain relievers and anti-diarrheal medications should be prescribed for their respective AEs.13
Early involvement of supportive and palliative care specialists can also be helpful in managing symptoms. The National Comprehensive Cancer Network (NCCN) guidelines provide further guidance for symptom management.14
FINANCIAL TOXICITY
Financial toxicity is increasingly relevant with use of novel drugs including PARPi for which there are no generic alternatives. This includes both out-of-pocket expenses such as the direct costs (co-pays, medications, co-insurance) and non-medical costs including transportation, lodging, childcare, and lost wages from time away from work.
Patients undergoing cancer treatments who are low income often spend up to 25% of their annual income on out-of-pocket medical costs.15 In addition, patients with cancer have a greater than two-fold higher risk of filing for bankruptcy compared to patients who do not have cancer, with nearly 60% of medically associated bankruptcies being due to cancer diagnoses.16
Financial toxicity has also been shown to negatively affect adherence to treatment.17 Though the oral formulation of PARPi allows patients to avoid costs associated with visits to the infusion center, it may come with a hidden cost due to a different level of insurance coverage.
For example, when olaparib was initially approved in 2017, the out-of-pocket cost was $12,585 per month without insurance, yet patients with insurance coverage still may pay over $2,000 per month.
Although there are medical assistance programs to help offset the cost of some PARPi, not all medical beneficiaries qualify.
New areas of investigation
PREDICTING RESPONSE
It has been well documented that tumors harboring germline or somatic BRCA mutations, and those that are “BRCA-like” with homologous recombination deficiency (HRD), tend to respond better to PARPi than their wild type counterparts.18,19
HRD positivity is seen in approximately 20% of patients with ovarian, fallopian tube, and primary peritoneal cancers who carry a germline mutation in BRCA1/BRCA2 or an associated cancer susceptibility gene such as RAD51C or RAD51D, and up to 50% of tumors.20
There are commercially available assays that can identify HRD-positive tumors among BRCA wild-type patients.
Anticipatory counseling about certain symptoms can reduce early discontinuation.
Interestingly, some studies have demonstrated efficacy of PARPi even in HR-proficient tumors, though the benefits are less pronounced in this population. Patients whose disease is still considered sensitive to platinum chemotherapy also appear to respond better to PARPi than those with platinum-resistant or -refractory disease.21
The mechanism is not fully understood and is an area for further inquiry.
MECHANISMS OF RESISTANCE
Multiple mechanisms of inherent or acquired resistance to PARPi have been identified and continue to be studied. These are complex mechanisms occurring at both the genomic and cellular levels and tend to disrupt the “synthetic lethality” effect that makes PARPi effective in susceptible cells with HRD.
One such mechanism is acquisition of BRCA reversion mutations which can restore BRCA protein function in BRCA-mutated tumors and make cells homologous recombination proficient.
With the HR pathway restored, cancer cells can repair DNA double-strand breaks that are induced by PARPi, thereby conferring a PARPi-resistant phenotype.
A recent study of patients with known germline or somatic BRCA mutations showed that detection of BRCA reversion mutations in circulating cell-free DNA prior to treatment was correlated with decreased progression-free survival and found more commonly among platinum-resistant or -refractory cancers.22
Used prospectively, this could become a means of choosing appropriate candidates prior to initiating PARPi therapy.
Another resistance mechanism that has been identified is upregulation of genes that encode for drug efflux pumps, which can lead to decreased intracellular levels of PARPi and thus less drug effect.23
Increased levels of proteins such as SLFN11 in tumors may augment the effects of PARPi, so low levels in tumors could eventually be used as a biomarker to predict PARPi resistance.24 Novel approaches are being developed to reverse resistance to PARPi by modulating these pathways.
MAINTENANCE THERAPY
Maintenance therapy is becoming ubiquitous in ovarian cancer care. The first FDA approval was in 2016, for the antiangiogenic agent bevacizumab after chemotherapy in patients with recurrent ovarian cancer.
Since then, bevacizumab has also been approved as frontline maintenance therapy, to be given after primary treatment. PARPi are now approved for use as maintenance in some patients in both settings (Table 1).
The question remains whether to administer maintenance therapy to all patients, and how to choose the most appropriate agent.
Table 1: Current FDA approvals for PARP inhibitor (PARPi) use in breast and ovarian cancer
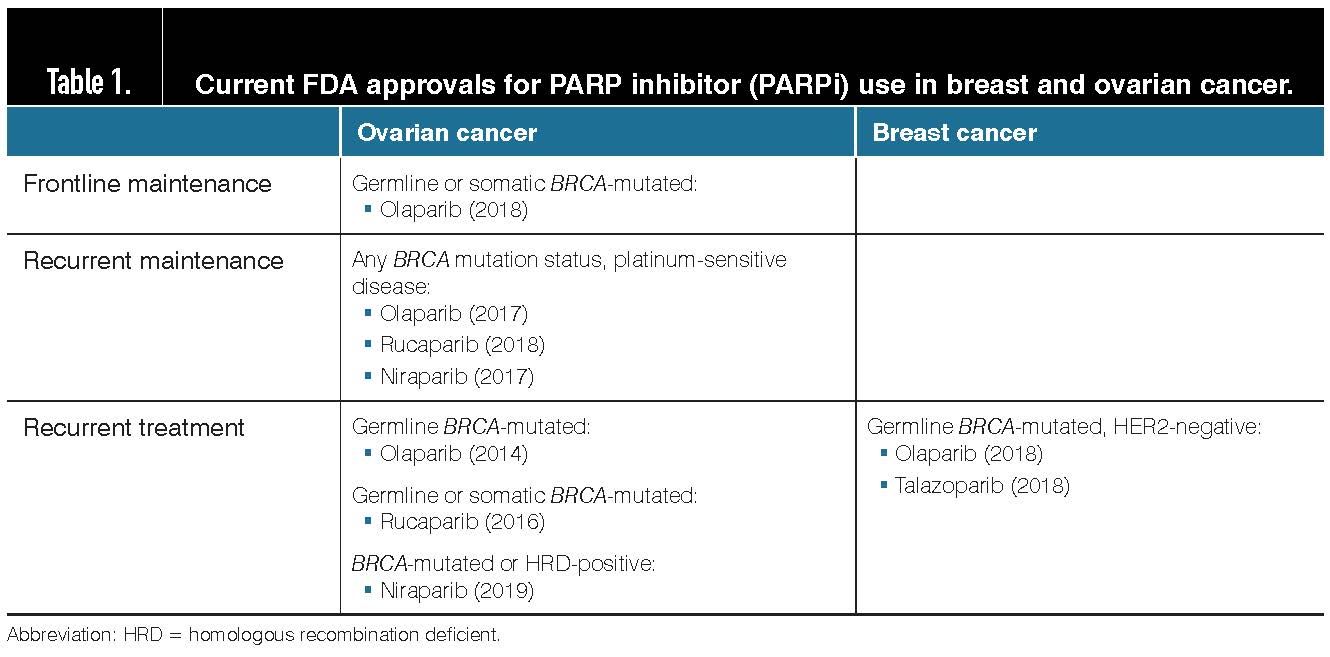
All three PARPi that are FDA-approved for use in ovarian cancer have indications for maintenance therapy in recurrent disease. Although these are irrespective of BRCA mutation or HRD tumor status, the magnitude of the benefit differs substantially by these factors, including sensitivity to the prior platinum chemotherapy treatment.
The number of disease-free months gained with PARPi use (compared to placebo) approaches 15 months in patients with a BRCA mutation, while this benefit is up to 9 months for those with HRD tumors and just 3 months in patients with HR-proficient disease (Table 2).9,10,25
Among PARPi, only olaparib is approved for frontline maintenance therapy, and is specifically for patients who harbor germline BRCA mutations. Veliparib and niraparib have been investigated in this setting as well with promising results, although the indication currently is not FDA-approved.
Interestingly, the combination of bevacizumab and olaparib as frontline maintenance led to significant prolongation of the disease-free interval for patients with BRCA mutations and HRD tumors.7
PARPI AFTER PRIOR PARPI USE
In the near future, many patients with recurrent ovarian cancer will have already been exposed to a PARPi as frontline maintenance therapy or as treatment for a prior breast cancer, and they could potentially be candidates for repeat PARPi use. Little is known about the efficacy and tolerability of PARPi in this setting.
The ongoing OReO trial (NCT03106987) is evaluating the potential benefit of repeat exposure to olaparib maintenance therapy in patients with recurrent, platinum-sensitive ovarian cancer who have previously been treated with olaparib, regardless of BRCA mutation status.
MOLTO (NCT02855697) is also investigating the impact of repeat olaparib exposure, but it is limited to patients with germline BRCA mutations.
Conclusion
With an abundance of recent data in ovarian cancer, the role of PARPi is rapidly evolving, and new standards of care are being developed. The paradigm for deciding which, if any, PARPi to give to a patient is complicated by the availability of bevacizumab as an alternative for maintenance therapy and traditional chemotherapy for treatment of recurrence.
Although the benefits of PARPi are clear in delaying disease recurrence among many patients with BRCA-mutated and HRD tumors, there is much to be learned about predictors of response and resistance to PARPi. Further, the associated cumulative AEs and their impact on overall survival is not yet known, and some patients and providers may be reluctant to use a PARPi for this reason.
Nonetheless, the addition of PARPi to the landscape of treatments for ovarian cancer represents an exciting breakthrough in the age of personalized medicine. Patients can safely be given PARPi for extended periods of time and maintain a high quality of life.
With knowledge of AE profiles, PARPi can be selected for a given patient based on her pre-existing symptoms and comorbidities, as these will impact the tolerability of specific PARPi.
Differential insurance coverage for each PARPi may further determine what is feasible for a given patient. With the anticipation of more FDA-approved indications for PARPi in ovarian cancer, it is hoped that these drugs can become more accessible to everyone.
Have your say online: Have you used PARPi to treat patients? What kind of success have you had using the treatment? What challenges have you encountered? Let us know on Twitter, Facebook, or by email.
References
1. Lynparza (olaparib) tablets [prescribing information]. Wilmington, DE: AstraZeneca Pharmaceuticals; December 2019.
2. Talzenna (talazoparib) [prescribing information]. New York, NY: Pfizer Labs; September 2019.
3. Zejula (niraparib) [prescribing information]. Waltham, MA: Tesaro; October 2019.
4. Rubraca (rucaparib) [prescribing information]. Boulder, CO: Clovis Oncology; April 2018.
5. Ledermann J, Harter P, Gourley C, et al. Olaparib maintenance therapy in platinum-sensitive relapsed ovarian cancer. N Engl J Med. 2012;366(15):1382-1392. 6. Moore KN, Secord AA, Geller MA, et al. Niraparib monotherapy for late-line treatment of ovarian cancer (QUADRA): a multicentre, open-label, single-arm, phase 2 trial. Lancet Oncol. 2019 May;20(5):636-648.
7. Ray-Coquard I, Pautier P, Pignata S, et al. Olaparib plus Bevacizumab as First-Line Maintenance in Ovarian Cancer. N Engl J Med. 2019;381(25):2416-2428.
8. Kristeleit R, Shapiro GI, Burris HA, et al. A Phase I–II study of the oral PARP inhibitor rucaparib in patients with germline BRCA1/2 -mutated ovarian carcinoma or other solid tumors. Clin Cancer Res. 2017 Aug;23(15):4095-4106.
9. Coleman RL, Oza AM, Lorusso D, et al. Rucaparib maintenance treatment for recurrent ovarian carcinoma after response to platinum therapy (ARIEL3): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet (London, England). 2017;390(10106):1949-1961.
10. Mirza MR, Monk BJ, Herrstedt J, et al. Niraparib Maintenance Therapy in Platinum-Sensitive, Recurrent Ovarian Cancer. N Engl J Med. 2016;375(22):2154-2164.
11. Coleman RL, Sill MW, Bell-McGuinn K, et al. A phase II evaluation of the potent, highly selective PARP inhibitor veliparib in the treatment of persistent or recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer in patients who carry a germline BRCA1 or BRCA2 mutation - An NRG Oncology/Gynecologic Oncology Group study. Gynecol Oncol. 2015;137(3):386-391.
12. de Bono J, Ramanathan RK, Mina L, et al. Phase I, dose-escalation, two-part trial of the PARP inhibitor talazoparib in patients with advanced germline BRCA1/2 mutations and selected sporadic cancers. Cancer Discov. 2017;7(6):620.
13. Moore KN, Monk BJ. Patient counseling and management of symptoms during olaparib therapy for recurrent ovarian cancer. Oncologist. 2016;21(8):954-963.
14. NCCN Clinical Practice Guidelines in Oncology. https://www.nccn.org/professionals/physician_gls/default.aspx#supportive.
15. Langa KM, Fendrick AM, Chernew ME, Kabeto MU, Paisley KL, Hayman JA. Out-of-pocket health-care expenditures among older americans with cancer. Value Heal. 2004;7(2):186-194.
16. Ramsey S, Blough D, Kirchhoff A, et al. Washington State Cancer patients found to be at greater risk for bankruptcy than people without a cancer diagnosis. Health Aff. 2013;32(6):1143-1152.
17. Doshi JA, Li P, Huo H, Pettit AR, Armstrong KA. Association of patient out-of-pocket costs with prescription abandonment and delay in fills of novel oral anticancer agents. J Clin Oncol. 2017;36(5):476-482.
18. Farmer H, McCabe N, Lord CJ, et al. Targeting the DNA repair defect in BRCA mutant cells as a therapeutic strategy. Nature. 2005;434(7035):917-921.
19. Watkins JA, Irshad S, Grigoriadis A, Tutt ANJ. Genomic scars as biomarkers of homologous recombination deficiency and drug response in breast and ovarian cancers. Breast Cancer Res. 2014;16(3):211.
20. Bell D, Berchuck A, Birrer M, et al. Integrated genomic analyses of ovarian carcinoma. Nature. 2011;474(7353):609-615.
21. Fong PC, Yap TA, Boss DS, et al. Poly(ADP)-ribose polymerase inhibition: frequent durable responses in BRCA Carrier ovarian cancer correlating with platinum-free interval. J Clin Oncol. 2010;28(15):2512-2519.
22. Lin KK, Harrell MI, Oza AM, et al. BRCA reversion mutations in circulating tumor DNA predict primary and acquired resistance to the PARP inhibitor rucaparib in high-grade ovarian carcinoma. Cancer Discov. 2019;9(2):210.
23. Lord CJ, Ashworth A. Mechanisms of resistance to therapies targeting BRCA-mutant cancers. Nat Med. 2013;19(11):1381-1388.
24. Murai J, Feng Y, Yu GK, et al. Resistance to PARP inhibitors by SLFN11 inactivation can be overcome by ATR inhibition. Oncotarget. 2016;7(47):76534-76550.
25. Pujade-Lauraine E, Ledermann JA, Selle F, et al. Olaparib tablets as maintenance therapy in patients with platinum-sensitive, relapsed ovarian cancer and a BRCA1/2 mutation (SOLO2/ENGOT-Ov21): a double-blind, randomised, placebo-controlled, phase 3 trial. Lancet Oncol. 2017;18(9):1274-1284.
Newsletter
Get the latest clinical updates, case studies, and expert commentary in obstetric and gynecologic care. Sign up now to stay informed.

