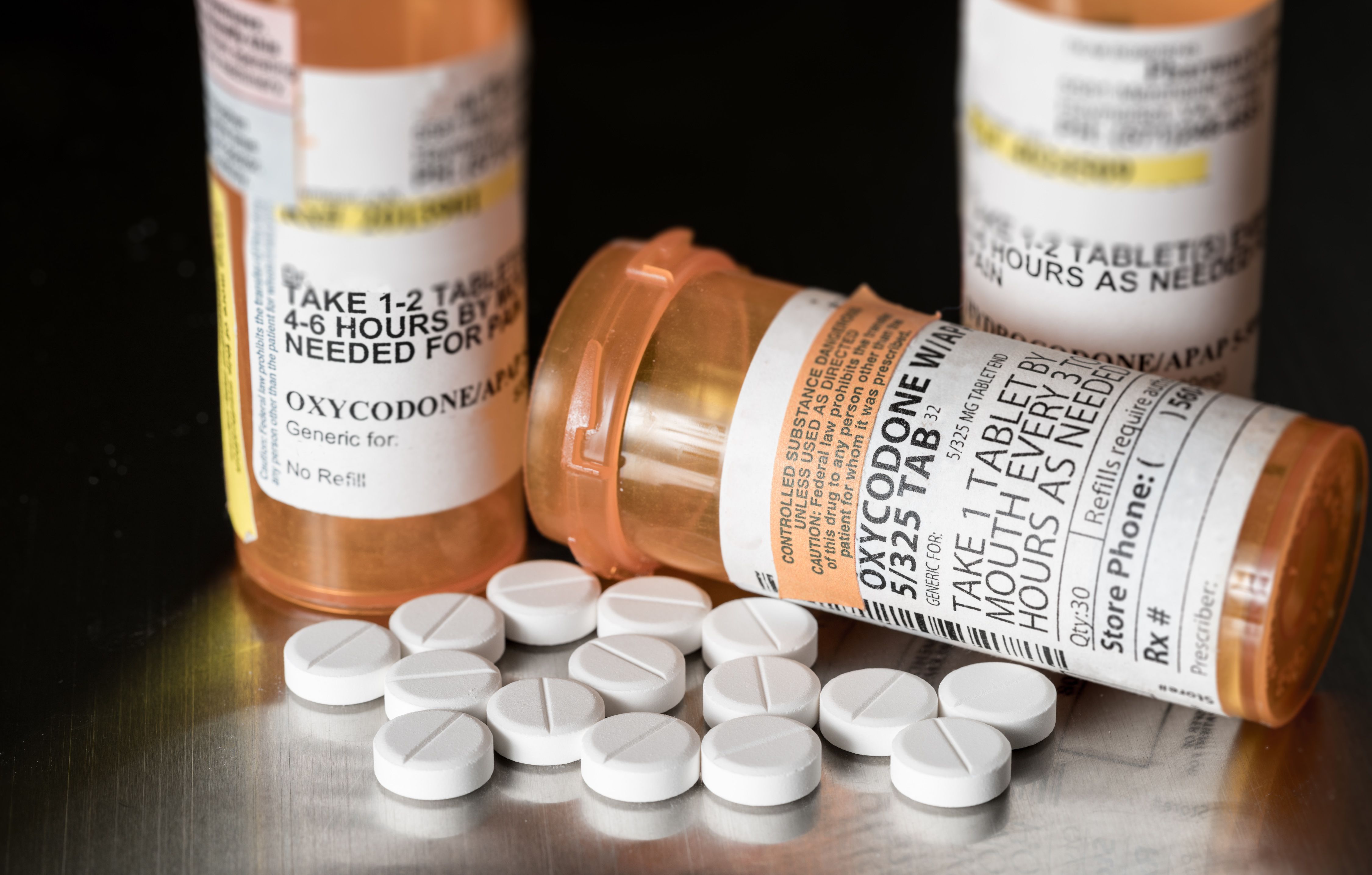
Total morphine milligram equivalents (MMEs) and number of opioid tablets at discharge following cesarean delivery are reduced by a personalized opioid prescription protocol, according to a recent study published in the American Journal of Obstetrics & Gynecology.
Takeaways
- Cesarean delivery is the most common surgery in the United States, yet there's no standard method for pain management upon discharge, leading to potential overprescription of opioids.
- A study proposes a personalized prescription protocol for post-cesarean pain management, aiming to reduce opioid prescriptions while ensuring adequate pain relief.
- Results show that the personalized protocol led to significantly lower morphine milligram equivalents prescribed at discharge compared to traditional methods, with fewer opioid tablets prescribed.
- Despite lower opioid prescriptions, patients in the personalized protocol group reported satisfactory pain management without needing additional opioid prescriptions.
- Implementation of a personalized prescription protocol nationwide could meaningfully reduce opioid overprescription following cesarean deliveries, addressing concerns of misuse, diversion, and addiction.
Over 1.1 million cesarean deliveries were performed in the United States in 2020, making it the most common surgery in the country. However, there is no standardized method for providing analgesia at discharge.
Recommendations from the American College of Obstetricians and Gynecologists Committee on Clinical Consensus-Obstetrics in 2021 suggest a stepwise multimodal approach including standard oral and parenteral analgesic adjuvants. Currently, pain management strategies prioritize the immediate postpartum period before discharge.
Data has indicated similar distribution of MMEs to patients following cesarean delivery regardless of pain before discharge. This has led to an excess of opioids, increasing the risks of misuse, diversion, and addiction. Therefore, a personalized prescription protocol may be necessary to decrease MMEs prescribed while still managing pain.
To evaluate the impact of a personalized prescription protocol on MME prescription, investigators conducted a prospective cohort study. Participants included pregnant individuals undergoing cesarean delivery at Parkland Hospital.
A traditional cohort included patients receiving the historical prescription of 30 tablets of acetaminophen-codeine 300/30 mg at discharge to take 1 to 2 of every 4 hours. These patients also took ibuprofen when necessary.
In comparison, patients in the personalized protocol cohort received 30 scheduled tablets of ibuprofen 800 mg and 100 tablets of acetaminophen 325 mg. These patients were also prescribed oxycodone tablets at discharge equal to 5 times the amount used in the previous 24 hours.
Data collection among the personalized cohort occurred from May 18, 2022, to June 29, 2022, vs March 21, 2021, to May 6, 2021, in the traditional cohort. Data was obtained from participants’ electronic medical records.
Relevant information included opioids received during hospital admission, opioid prescription at discharge, number of opioids prescribed, and if the prescription was filled. Total MMEs prescribed at discharge was reported as the primary outcome of the analysis, while the number of tablets at discharge was reported as a secondary outcome.
There were 412 patients in the personalized cohort and 367 in the traditional cohort included in the analysis. Race, parity, and body mass index did not differ between these groups.
The MMEs used while inpatient were greater in the personalized cohort, but the median MMEs prescribed at discharge were lower in this group, at 37.5 vs 135 in the traditional cohort. An opioid prescription was reported in 100% of the traditional cohort vs 57% of the personalized cohort.
Of the 57% of patients in the personalized cohort who received opioid prescriptions, 11% did not fill the prescription. The prescription status could not be confirmed in 8%. A hotline phone call was reported by 2.2% of the personalized cohort, none of whom required a rescue course of opioids for analgesia after a trial of ibuprofen.
Presenting to the emergency department with a primary complaint of pain was reported in 1.6% of the traditional cohort vs 2.7% of the personalized cohort. No patients in either cohort needed readmission or outpatient opioid prescription.
These results indicated decreased MME prescriptions following discharge for cesarean delivery when utilizing a personalized prescribing protocol. Investigators concluded national implementation of a personalized prescribing protocol would lead to a meaningful impact.
Reference
Imo CS, Macias DA, McIntire DD, et al. A personalized protocol for prescribing opioids after cesarean delivery: leveraging the electronic medical record to reduce outpatient opioid prescriptions. Am J Obstet Gynecol. 2024;230:446.e1-6. doi:10.1016/j.ajog.2023.09.092