Solutions for spinal headaches
Curbside Consults delivers expert perspectives from physicians outside the ob-gyn specialty to provide insight into various health issues affecting pregnant women. In this installment, we learn more about the diagnosis and management of headaches in postpartum patients.
A healthy 26-year-old gravida 1, para 1 (G1P1) female is postpartum day 1 after a term spontaneous vaginal delivery. Her labor pain was reduced through the use of an epidural catheter and placement was unremarkable with no indication of an inadvertent dual puncture.
Twelve hours after delivery, she began to complain of a severe headache. She described the headache as dull, throbbing, and significantly worse when she tried to walk around her room. She also felt nauseated and described experiencing double vision when she sat up.
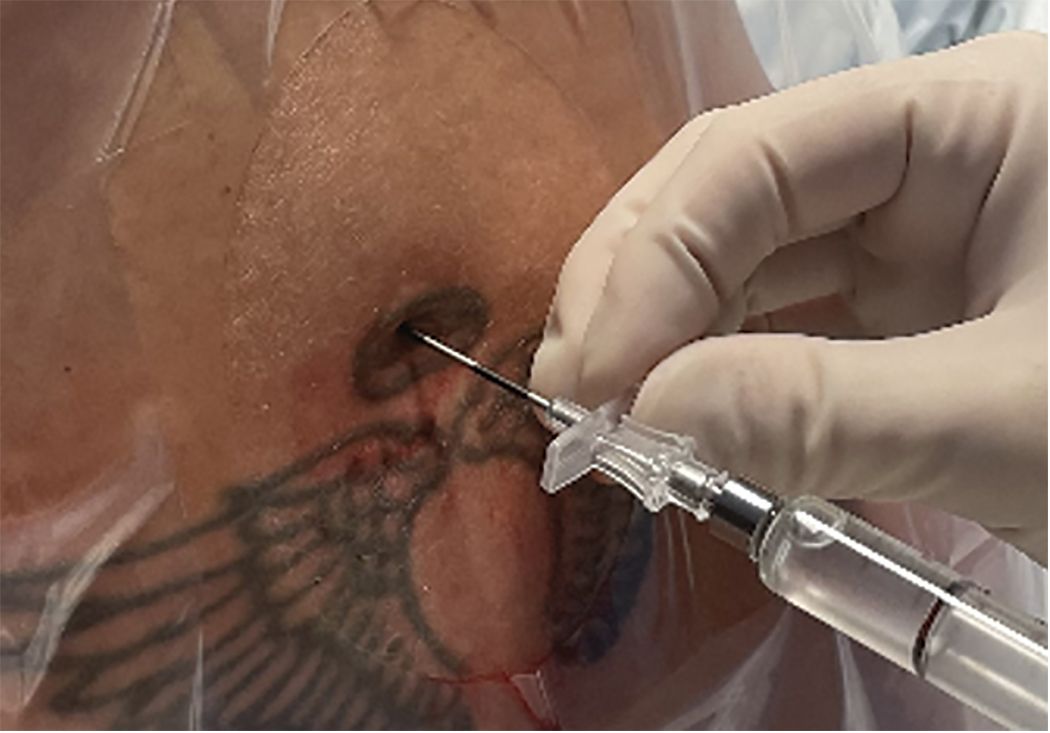
Additionally, she had severe neck pain and stiffness. Her symptoms were slightly improved by lying down. She complained of accompanying photophobia(Figure 1).
Figure 1. Sample image of an epidural placement with a 17-gauge Tuohy needle and attached glass syringe.
Background
The diagnosis and management of headaches in the postpartum patient is a frequently encountered situation for the ob-gyn physician. In fact, 39% of women report having a headache within 1 week after giving birth.1
These headaches vary in onset, cause, and treatment modality, and it is not uncommon for the obstetrician to be the first provider to discover their patient’s headache after delivery.
Because of this and given the nature of labor analgesia via neuraxial block in modern-day peripartum care, it is increasingly important for obstetricians to have a more in-depth understanding of the postdural puncture headache (PDPH).
A PDPH, also known as a spinal headache, occurs in 6% to 36% of all neuraxial procedures, but only in about 1% of all neuraxial blocks on the labor and delivery floor.1 The headache is caused by a slow cerebrospinal fluid (CSF) leak through a defect in the meninges, causing intracranial hypotension with resultant traction on pain-sensitive structures and reactive venodilatation.2
In other words, a hole in the dura mater in the lumbar spine allows CSF to leak out, causing the brain to lose its cushion and the sag in the skull resulting in painful headaches from venous traction and dilation.
Several patient factors can increase the risk of a PDPH, including female gender, pregnancy, lower body mass index, and a history of headaches.2 Furthermore, vaginal delivery and excessive pushing during labor can increase the risk of a spinal headache after a postdural puncture.
Provider factors can also elevate the risk of PDPH and include inexperience with epidurals and an increased number of attempts made at placing the neuraxial block.
The type and size of needle used for dural puncture also influences the prevalence of PDPH, with Tuohy needles and cutting/traumatic spinal needles being more likely to cause a PDPH than nontraumatic/pencil point spinal needles.
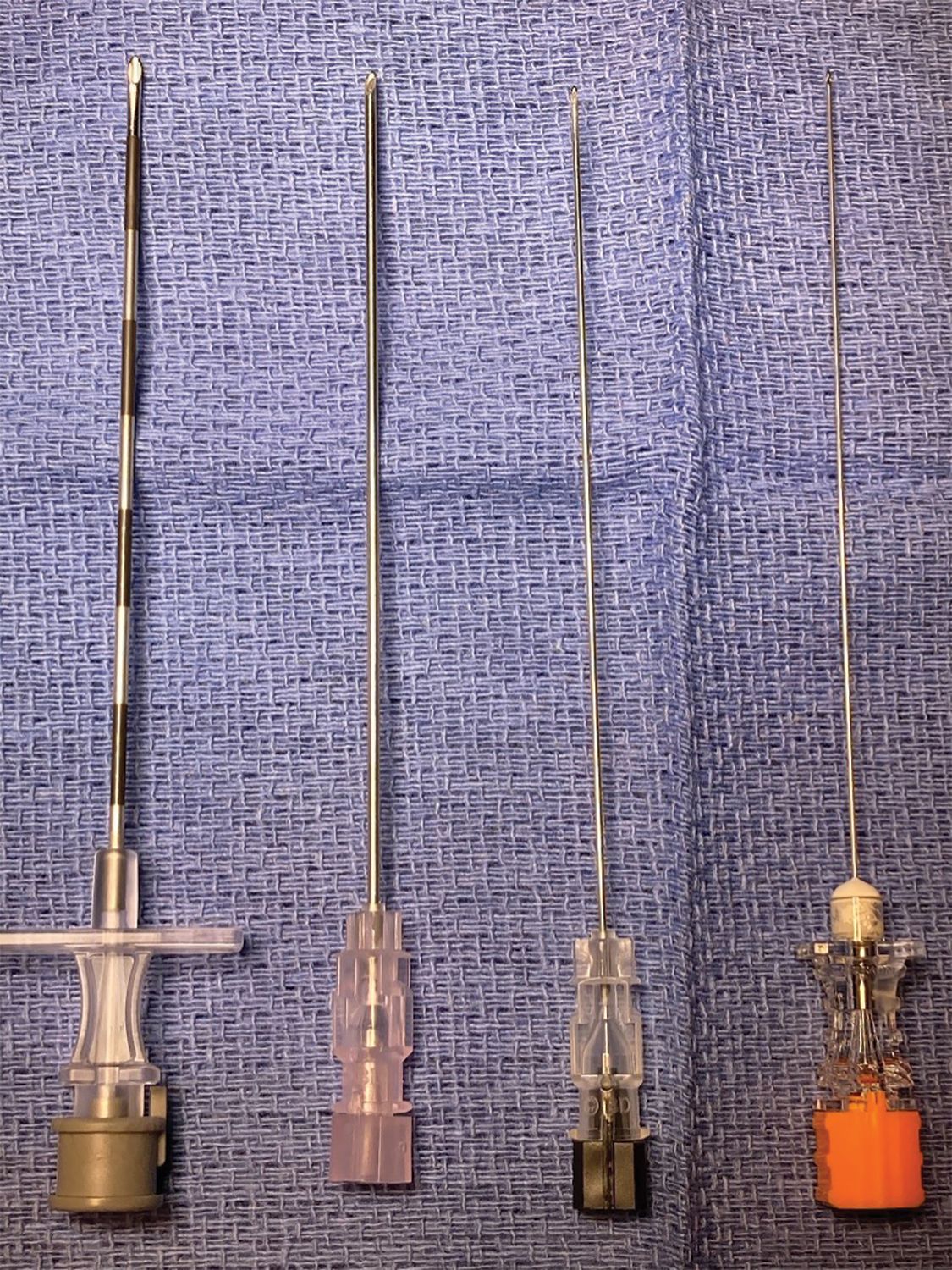
Notice the difference in diameter of the needles in the photo (Figure 2).
The largest, the Tuohy, is a 17-gauge needle. The smallest needle is known as a Pencan and is a 25-gauge needle.2
Figure 2. Neuraxial needles of different sizes.
A 17-gauge Tuohy needle (left) is used to enter the epidural space. The additional needles are spinal needles of 18-, 22-, and 25-gauge, respectively. The larger the needle that traverses the dura, the greater the likelihood that the patient will develop a PDPH. Typically, 25-gauge spinal needles are used in obstetrics anesthesia.
Presentation
Patients with PDPH will most often present with a dull or throbbing headache that is bilateral, occipital-frontal in location, and of varying severity.
The true hallmark of this condition is a change in the severity of the headache with patient positioning.
These patients will have worsening symptoms after standing or sitting for 15 minutes and should feel an improvement after lying down for 15 minutes.2 Their symptoms may be worsened with coughing or straining. In greater than 50% of cases, patients will have associated symptoms of nausea, photophobia, tinnitus, vertigo, or diplopia.1
The symptoms that patients with PDPH experience are the result of the meninges and cranial nerves being stretched as these structures sag due to the decreased volume of the CSF. Patients who are unable to function and care for their baby due to debilitating symptoms should be considered for an epidural blood patch (EBP).
It is best to have patients come to the labor and delivery department to be evaluated and avoid having them wait in the emergency department for hours.
Initial management by an obstetrician
Patients who present with mild PDPH without associated symptoms can often be treated conservatively without the need for intervention by an anesthesiologist.
Figure 3. Sample image of a Tuohy needle in the lumbar epidural space during placement of an epidural blood patch.
First-line analgesics include oral or IV nonsteroidal anti-inflammatory medications. Hydration with IV fluids and IV caffeine reduces the need for supplementary conservative interventions and should be the cornerstone of addressing patients with mild PDPH.3
Other medications such as theophylline, gabapentin, and hydrocortisone have all been shown to reduce pain scores.3
In the event of failed conservative management or severe symptoms with associated sequelae, an anesthesiologist can be consulted to perform a regional nerve block or an EBP. The EBP is an aseptic collection and injection of autologous blood into the epidural space. The blood creates a seal to the dural puncture, preventing further CSF leak.1
Essentially, the anesthesiologist repeats the epidural process (Figure 3), injecting sterile blood into the epidural space to form a “patch” among the injured dura mater. Patients with successful blood patches will have immediate symptomatic relief during the procedure, with cessation of the headache being one of the positive endpoints.
If the procedure is not successful, it can be repeated at the discretion of the anesthesiologist after 24 hours have elapsed from the first EBP. Patients can be discharged home following the placement of EBP.
References
- FitzGerald S, Salman M. Postdural puncture headache in obstetric patients. Br J Gen Pract. 2019;69(681):207-208. doi:10.3399/bjgp19X702125
- Patel R, Urits I, Orhurhu V, et al. A comprehensive update on the treatment and management of postdural puncture headache. Curr Pain Headache Rep. 2020;24(6):24. doi:10.1007/s11916-020-00860-0
- Basurto Ona X, Osorio D, Bonfill Cosp X. Drug therapy for treating post-dural puncture headache. Cochrane Database Syst Rev. 2015;(7):CD007887. doi:10.1002/14651858.CD007887.pub3

Newsletter
Get the latest clinical updates, case studies, and expert commentary in obstetric and gynecologic care. Sign up now to stay informed.
S4E1: New RNA platform can predict pregnancy complications
February 11th 2022In this episode of Pap Talk, Contemporary OB/GYN® sat down with Maneesh Jain, CEO of Mirvie, and Michal Elovitz, MD, chief medical advisor at Mirvie, a new RNA platform that is able to predict pregnancy complications by revealing the biology of each pregnancy. They discussed recently published data regarding the platform's ability to predict preeclampsia and preterm birth.
Listen
