
Interview with Steve Fleischman

Interview with Steve Fleischman

Roberta Speyer: “This is Roberta Speyer and I’m reporting for OBGYN.net. I have the pleasure of talking to Dr. Fleischman who is an Assistant Clinical Professor at Yale University and in private practice with Gynecology & Infertility, PC. Today we are going to talk about urinary incontinence and how OBGYN physicians can fit this into their practice. As a practicing OBGYN yourself, this is something you have a great degree of specialization in. Tell us a little about your practice Dr. Fleischman.”

The average age of natural menopause in Western societies is estimated to be 51 years; women in Canada can therefore expect to live, on average, a third of their lives in post-menopausal years. During these years women are at increased risk of chronic diseases such as osteoporosis and cardiovascular disease.

Researchers from Italy have found that premenopausal breast cancer patients treated with triptorelin and chemotherapy were less likely to experience early menopause and were more likely to resume menses than patients who received chemotherapy alone.

Thanks to innovative treatments like in vitro fertilization and egg donation, we are able to help thousands of infertile patients build their families.

The use of chemotherapy for the treatment of breast cancer can result in transient or permanent amenorrhea, and research indicates that each month of chemotherapy translates into 1.5 year of lost reproductive life. This is especially significant for women younger than 40 years, which accounts for 6% of the population diagnosed with breast cancer.

This is the exercise which, when done faithfully and correctly, can help decrease the urgency a patient may have and help with both urge incontinence and stress incontinence. The pelvic floor muscle is like a hammock that stretches from the pubic bone in the front to the tailbone in the back.

The age at which a woman reaches menopause is 85% genetically determined, according to new research published Thursday, in Europe's leading reproductive medicine journal, Human Reproduction*.

Many risk factors for fractures have been documented, including low bone-mineral density (BMD) and a history of fractures.

In an extensive, multi-center clinical treatment trial, Canadian researchers evaluated the outcomes of 538 cases of uterine artery embolization for fibroids. Between 20% and 50% of women develop uterine fibroids, benign tumors in the muscular tissue of the uterus that can seriously impact their health and well-being.

Ovulation induction is based on the administration of gonadotropins in order to enhance fertility. Daily administration of the drug causes a supra-physiological increase in serum FSH leading to the recruitment of a larger cohort of follicles, further causes their growth and development, and finally, triggering ovulation of usually more than one follicle.

The oviduct is an exquisitely designed organ that functions in picking-up ovulated oocytes, transporting gametes in opposite directions to the site of fertilization, providing a suitable environment for fertilization and early development, and transporting preimplantation embryos to the uterus.

Women with cystic fibrosis can have fertility treatment to help them have babies without any long-term adverse effects on either themselves or their children, according to new research presented at the 25th annual meeting of the European Society of Human Reproduction and Embryology in Amsterdam today (Tuesday).

Women who have a diminished number of eggs in their ovaries, either because they are older or for some other reason such as ovarian surgery, may be more at risk of a trisomic pregnancy than women with an ovarian reserve within the normal, fertile range.

One-step screening for both genetic and chromosomal abnormalities has come a stage closer as scientists announced that an embryo test they have been developing has successfully screened cells taken from spare embryos that were known to have cystic fibrosis.

Transferring just one embryo at a time to a woman’s womb after embryos have undergone preimplantation genetic diagnosis (PGD) and freezing at the blastocyst stage has become a real option after researchers achieved pregnancy rates that were as good as those for blastocysts that had not had a cell removed for PGD before freezing.

A new test examining chromosomes in human eggs a few hours after fertilisation can identify those that are capable of forming a healthy baby, a researcher told the 25th annual conference of the European Society of Human Reproduction and Embryology on 29 June.

A new technique for transplanting the ovaries of women who have lost their fertility as a result of cancer treatment was outlined to the 25th annual conference of the European Society of Human Reproduction and Embryology on Monday 29 June.

Analysis of the longest running ICSI programme in the United States has found reassuring evidence that babies born from frozen embryos fertilised via ICSI (intracytoplasmic sperm injection) do just as well as those born from frozen embryos fertilised via standard IVF treatment.

The largest study to date of endometriosis in pregnant women has found that the condition is a major risk factor for premature birth, the 25th annual conference of the European Society of Human Reproduction and Embryology heard today (Wednesday July 1).

Until now there has been no evidence-based consensus amongst fertility specialists as to whether or not men should refrain from sex for a few days before attempting to conceive with their partner, either spontaneously or via assisted reproduction.

Comments from Specialists I heard from a reliable newspaper or television station that he implanted 6 and two of the embryos split into twins. Allen Worrall, RDMS Intra - endometrial implantation is evolving to be a superior method and Dr Kamrava deserves recognition for this contribution but......if hysteroscopic embryo implantation is supposed to be 70% more effective than the "blind technique", why then would Dr Kamrava aim to obtain 8 pregnancies??????George Haber, MD Regardless of the media hype and not knowing the inside story of why so many embryos were implanted, we have apparently a high success rate technique with zero ectopics, this is worth considering. Let's separate science from entertainment.Mario E. Domenzain, M.D., F.A.C.O.G. What we so far know about implantation is that it is a very complex process, where a sequence of events happens with a very delicate synchronization (selection of the site of implantation by Selectin molecules which help the blastocyst "roll" to the right spot, MUC-1 repelling it from the "bad" ones, chemokines and cytokines -LIF, IL-1. Integrins- attracting it, adhesion molecules attaching it to pinopodes, to cite a few). I doubt that forcibly "implanting" an embryo into a self-selected spot in the endometrium could really improve pregnancy rates; it is bypassing the natural selection process (for example: embryos do not "take" on endometrium without pinopodes either because of poor timing or because of endometrium defect). Hysteroscopic embryo implantation might reduce the rate for ectopic pregnancies. But unless the hysteroscopic process in itself stimulates the release of these molecules on the spot (like the repeated Pipelle might be doing???), it should not improve the overall pregnancy rate. I of course -and all my IVF team in Jerusalem, where we do see several very religious women "pushing" for many children!!!, cannot agree with replacing 8 embryos by ANY type of woman (especially if she is young and proven fertile !!!!) Dr Hava-Yael Schreiber, M.DOB/GYN and Fertility specialist Zir Chemed Medical Center and Bikur Holim Hospital, Jerusalem Roberta and friends, There has been such a media frenzy about this, and for good reason. While any licensed practitioner is theoretically entitled to their own opinion about procedures, standard of care dictates the concept of evidence-based medicine, i.e. do no harm and do what is reasonable based on the best interpretation of peer-reviewed medical literature. When Dr. Kavarna gave this interview awhile ago, perhaps he had a hypothesis that hysteroscopic assistance of embryo transfers would aid the success of implantation. To my knowledge, he hasn't proven the value of this technique, nor has anyone else. And in fact, the standard of care has become ultrasound-assisted embryo transfer, which is hardly a blind technique. In fact, many centers (such as ours) utilize echo-tip catheters which allow for excellent visualization of transfer catheter placement via abdominal ultrasound, especially when the patient has a moderately full bladder. Now as far as results, prospective patients who are looking into IVF, along with their physicians, should be strongly urged to evaluate data published annually online by the Society for Assisted Reproductive Technology (SART) at www.sart.org Although there is a lag in SART's ability to compile and post data, both patients and physicians can get an idea of who is doing what, practice-by-practice, and both nationally and regionally. Currently, the latest data listed on the SART website is from 2006, but I believe 2007 will be available soon. Most SART clinics have already compiled preliminary 2008 data but have not yet submitted, mainly because final results are not in yet for live births generated from 2008 cycles. Now, you asked about our data. And here is what I can share, which is available already publicly (2006) and will soon be available publicly (2007): For women under 35 using fresh non-donor eggs, the live birth rate per transfer in 2006 was 51.4 percent, and we transferred an average of 1.8 embryos for those patients. For that group, 22.2 percent had elective single embryo transfer. The overall implantation rate was 43.1% (see https://www.sartcorsonline.com/rptCSR_PublicMultYear.aspx?ClinicPKID=2442 for the full summary) In 2007 for the same group, the live birth rate per transfer was 55.1%, and we transferred an average of 1.4 embryos. Approximately 60% of our patients < 35 had a single embryo transfer. SART calculates the implantation rate after the data is submitted, but I would estimate it to be around 45-50%. This trend towards "fewer is better" is again seen in our preliminary 2008 results. We had an abstract at ASRM in 2007 which also concluded this, based on the results we had at that time. There is so much focus these days on clinics that are doing a substandard job, I think it's time for the media to infuse some hope into those who could benefit from great fertility care, and by letting people know there are some centers that are exceeding national averages and have the data to prove it. There are many important factors that go into generating high success rates, and I'm happy to discuss this further with anyone in the media who might be interested. Regards to all,Ronald F. Feinberg MD, PhDIVF Medical Director Reproductive Associates of Delaware Suite 3217, Medical Arts Pavilion 2 4735 Ogletown-Stanton Road Newark, DE 19713 302-623-4242 FAX 302-623-4241www.ivf-de.org "The ethical, personal care that helps families grow." Dear Editor of Ob-Gyn Net: I was appalled and saddened when I heard that a physician had intentionally transferred multiple embryos into a woman who had already had a multiples birth. This showed very poor judgment, in my opinion. It is also contrary to the guidelines of SART for infertility clinics. Because of all of the potential problems for these ultra-light babies, now and in the future, it is against the ethical principle of justice or “community good”. I am sure the California Board of Medical Examiners will be looking into this and well they should. The public is rightly infuriated over this situation and should demand an investigation by the Board if it is not forthcoming. Even the old caution that doctors have tried to follow for centuries, “primum non-nocere”, first, do no harm, has been breached. This whole situation likely will result in new laws or requirements for REIs and clinics that specialize in infertility. Thomas F. Purdon, MD FACOG No need to apologize. Many of us were curious about this individual, and you gave us what you had. I didn't see it as flashy or trashy--it was a legitimate interview about a relevant topic. Remember, curious people want to know.Steven Nelson MDPhoenix, AZ Dear Madam: Greetings! The interview was done as if we are condoning this procedure. Maybe this is becoming a moral issue like doctors playing God. Yes the interview was done in poor taste the interviewer allowing himself to be manipulated. Thank you and more power.Dr. Ferry AnolinManila, Phillipines I think it sounds like a very innovative procedure that may improve outcomes. (Obviously using only 1 or 2 embryos) Ginger H. Riley

A substantial number of European patients travel to other countries for fertility treatment, both because they think that they will receive better quality care abroad and in order to undergo procedures that are banned in their home country says a study of the subject launched at the 25th annual conference of the European Society of Human Reproduction and Embryology today (Monday June 29).
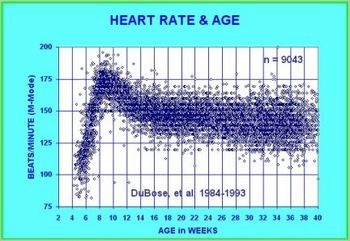
The embryonic heart rate (EHR) has been found to correlate with gestational age by crown-rump length (CRL) in normal pregnancies. This research compares the EHR and CRL for a population (n=173) in an assisted fertility program, and a population (n=173) of normal pregnancies which were paired by CRLs.

There are many factors that go into the decision to choose a birth control method. This article is intended to be an overview to help you to think about these choices, and make a decision about what method is best for you.