2019 ASCCP guidelines: Pearls for practitioners
Consensus group discussion resulted in a shift from results-based to risk-based management for cervical cancer screening.
Rebecca Perkins is an associate professor of obstetrics and gynecology at Boston University School of Medicine and Boston Medical Center in Massachusetts. She was cochair and one of the lead authors of the 2019 ASCCP Risk-Based Management Consensus Guidelines. Her career is dedicated to reducing health disparities in cervical cancer.

Increased knowledge of the natural history of human papillomavirus (HPV) infection has allowed the evolution of guidelines for cervical cancer screening and management of abnormal results. From 2017 to 2019, a consensus group that included 19 national organizations involved in cervical cancer prevention met to revise guidelines for managing abnormal cervical cancer screening test results and cancer precursors. The result was a paradigm shift from results-based management to risk-based management.1
The concept of risk-based management means that patients are managed based on their risk of having severe precancer (cervical intraepithelial neoplasia [CIN] grade 3 positive) or cancer, rather than solely on specific test results. Correct application of these guidelines will lead to less aggressive treatment for low-risk patients and more aggressive treatment for high-risk patients. Modeling studies indicate that adopting these guidelines will be cost-effective and save lives.2
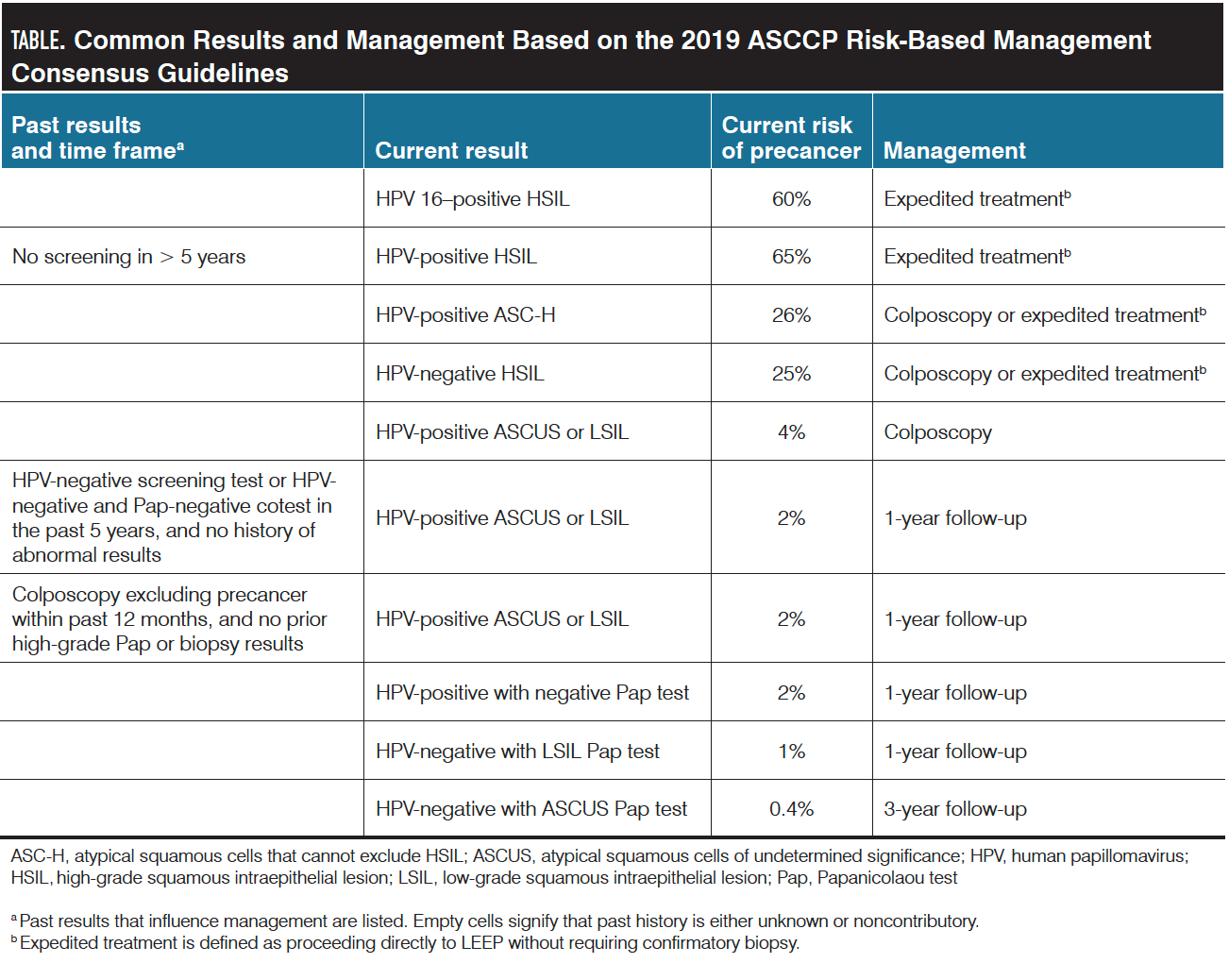
Table. Common Results and Management Based on the 2019 ASCCP Risk-Based Management Consensus Guidelines
ASC-H, atypical squamous cells that cannot exclude HSIL; ASCUS, atypical squamous cells of undetermined significance; HPV, human papillomavirus; HSIL,high-grade squamous intraepithelial lesion; LSIL, low-grade squamous intraepithelial lesion; Pap, Papanicolaou test
a. Past results that influence management are listed. Empty cells signify that past history is either unknown or noncontributory.
b. Expedited treatment is defined as proceeding directly to LEEP without requiring confirmatory biopsy.
The guidelines (Table) are complex because they encompass nuances of history and current results. Trying to understand the multitude of small differences can seem overwhelming to clinicians. However, there are a few changes that are most crucial, which will be reviewed below.
1. HPV testing is necessary for proper management.
Because HPV infections cause nearly all cervical cancers, HPV testing is a key component of care. More precise management is possible when patients are tested using either HPV testing alone or cotesting (simultaneous HPV and Papanicolaou [Pap] testing). The American Cancer Society now recommends initiating screening at age 25, with HPV testing alone.3 The US Preventive Services Task Force and American College of Obstetricians and Gynecologists recommend HPV testing or cotesting for patients 30 years and over.4,5 Although Pap testing alone is allowed for screening in these guidelines, HPV testing or cotesting is preferred for patients who have had an abnormal result.
2. Clinical decision support tools are the best way to manage patients.
Because of the complexity of incorporating both history and current test results to obtain precise risk estimates, using a clinical decision support tool is the easiest way to ensure you are following guidelines with your patients. The American Society for Colposcopy and Cervical Pathology (ASCCP) has a phone-based app for purchase and a free web version for providers.6 A free patient-facing tool, including education on why a particular management is recommended, is also available from Boston Medical Center.7
3. Patients who are extremely high risk for (severe) precancer (CIN 3 positive) can proceed directly to treatment without requiring a confirmatory biopsy.
Patients whose current risk of precancer (CIN 3 positive) is 60% or higher may proceed directly to excisional treatment with a loop electrosurgical excision procedure (LEEP) without requiring a confirmatory biopsy first. This is called expedited treatment. Expedited treatment lessens the risk of missing lesions at colposcopy and minimizes the number of visits for patients, which reduces loss to follow-up. The LEEP provides both diagnosis and treatment in a single visit. An examination using a colposcope and acetic acid is usually performed at the time of the LEEP procedure to ensure there is a visible lesion to excise and to rule out invasive cancer. If there is a concern for cancer, biopsies should be taken. Reasons to avoid proceeding directly to LEEP are if a patient is pregnant or if a LEEP is not readily available, which would delay diagnosis. It is important not to delay diagnosis, as up to 8% of patients with these results may have cancer.1 Result combinations that warrant LEEP treatment without prior biopsy are:
(1) HPV test that is positive for type 16, accompanied by a high-grade squamous intraepithelial lesion (HSIL) on Pap test; and
(2) HPV-positive HSIL on Pap test (regardless of HPV high-risk genotype) in patients who have not been screened in over 5 years.
4. Patients who are at moderate risk for precancer (CIN 3 positive or CIN 2-3) may elect to undergo LEEP treatment (expedited treatment) or colposcopy.
Patients whose current risk of precancer is between 25% and 59% may elect to undergo a LEEP instead of a colposcopy with biopsy (ie, expedited treatment). Results that fall into this category include HPV-positive atypical squamous cells that cannot exclude HSIL (ASC-H) and HPV-negative HSIL. This option may be particularly useful in patients who have completed childbearing, who have had several years of abnormal Pap and/or HPV tests, and whose Pap test results have been slowly worsening but lesions have not been detected on past colposcopies.
5. Colposcopy with biopsy is always required for certain results.
A tissue diagnosis, usually colposcopy with biopsy, is always required when HPV 16 or 18 is detected, and for high-grade Pap test results including HSIL, ASC-H, and atypical glandular cells. Colposcopy is also required if a patient has 2 consecutive HPV-positive results. In the case of HPV 16-positive HSIL, described above, the patient may be directly treated and receive the tissue diagnosis from the LEEP specimen rather than a colposcopic biopsy.
6. Colposcopy should be performed according to the colposcopy standards.8
Colposcopy is used to identify or exclude a precancerous lesion (CIN2, CIN3, histologic HSIL, or adenocarcinoma in situ). To ensure severe precancers (CIN 3 positive) are detected, all acetowhite lesions should be biopsied, usually 2 to
4 biopsies per patient.8 If no lesions are visible, an endocervical curettage should be performed.9
7. Patients with a history of negative HPV tests or cotests with a new low-grade abnormal result can follow up in 1 year instead of having a colposcopy.
Patients who do not have a history of abnormal results and whose last screening results were a negative HPV test or cotest within the past 5 years (ie, performed at the recommended screening interval) are at low risk for precancer. This allows colposcopy to be deferred for certain low-risk results. Specifically, a patient can return in 1 year instead of proceeding directly to colposcopy if they have a new HPV-positive low-grade squamous intraepithelial lesion (LSIL) or HPV-positive atypical squamous cells of undetermined significance (ASCUS) preceded by a negative screening HPV test or cotest (provided they do not have prior abnormal results). The prior negative HPV testing reduces their current risk of precancer from 4% to 2%, which is below the 4% risk threshold for which colposcopy is recommended.1
8. Patients with a persistent low-grade abnormal result on a screening and a colposcopy can now undergo colposcopy every 2 years.
Some patients are caught in a cycle of repeated low-grade abnormal results and low-grade colposcopy findings. Previously, colposcopy was recommended for these patients every year. However, data indicate that the risk of precancer with an HPV-positive ASCUS or LSIL result falls from 4% to 2% if a patient had a normal colposcopy within the past year (provided there is no history of high-grade results). Therefore, the recommendation in this situation is to repeat the HPV test or cotest in 1 year instead of performing a colposcopy. If the patient continues to have abnormal results at the 1-year follow-up, colposcopy is recommended at that time. In this scenario, surveillance with HPV testing or cotesting occurs annually, and for patients who continue to have persistently low-grade abnormal results, colposcopy is performed every 2 years instead of every year. This is helpful to reduce the number of colposcopies performed on patients with persistent low-grade results for whom precancers are not found.
9. Surveillance is required for at least 7 years after low-grade abnormal results before a patient can return to routine screening.
Following low-grade abnormal results, close-interval follow-up is recommended to ensure resolution of the problem before returning a patient to a routine (5-year) screening interval. For patients with a low-grade result, such as HPV-positive ASCUS or LSIL followed by a colposcopy excluding precancer, follow-up with HPV testing or cotesting is recommended at 1 year. If this result is normal, the patient may be followed every 3 years until 3 consecutive negative HPV tests or cotests have been obtained prior to returning to a 5-year interval. This totals 7 years of follow-up because of the initial abnormality and colposcopy, the first follow-up 1 year later, then 2 additional tests at
3-year intervals.
10. Surveillance is required for 25 years after high-grade abnormal results before the patient can return to routine screening.
After a patient receives a diagnosis of precancer (eg, CIN2, CIN3, or histologic HSIL), annual HPV testing or cotesting is recommended for 3 consecutive negative tests. After this, the testing interval can be extended to 3 years. Patients should continue testing with HPV testing or cotesting every 3 years for 25 years before returning to a 5-year interval. Testing should continue even if the patient undergoes hysterectomy or becomes older than 65 during this period. Patients with a history of precancer appear to remain at elevated risk for invasive cancer for a minimum of 25 years, and possibly longer, so continuing screening beyond 25 years if the patient is older than 65 and in good health is an option.
11. Persistent CIN1 should be observed, not treated.
A histologic diagnosis of CIN1 is a marker of an active HPV infection but does not indicate precancer. For this reason, continued observation of CIN1 is recommended rather than treatment. Treatment is an option if strongly desired by the patient.
12. Patients requiring follow-up in 1 year should be actively managed to ensure they do not miss their follow-up.
Annual Pap tests were previously the standard of care, and many patients regard a 1-year interval as normal. However, in the new screening and management guidelines, a 1-year follow-up is recommended for patients who have a low risk of precancer (0.6% to 3.0%) compared with those with negative screening tests (0.1%). New guidelines that recommend deferring colposcopy for low-grade results (see 7 and 8) rely on the 1-year follow-up test to detect new lesions. Therefore, patients requiring 1-year follow-up should be actively tracked by medical staff.
13. Patients with symptoms concerning for cervical cancer should have Pap and HPV tests as part of their evaluation, even if they are not due for screening.
By definition, screening tests are performed on asymptomatic patients. If a patient presents with symptoms concerning for cervical cancer, such as postcoital bleeding or abnormal uterine or vaginal bleeding, a Pap and HPV test should be performed as part of the diagnostic work-up. Although cancers are rare among screened patients, failure to perform adequate diagnostic testing in the setting of symptoms can delay diagnosis and worsen prognosis.
14. The best way to prevent cervical cancer is to ensure adequate screening.
Recent data indicate that 60% of women who developed cervical cancer had not been screened in over 5 years and 22% had not received adequate follow-up on an abnormal result.10 Thus, 82% of cancers would be preventable with adequate screening and follow-up. Recent data indicate that more cancers were diagnosed at later stages, leading to a decrease in overall cervical cancer survival from 64% to 62% between 2003 and 2014.11 In addition, only one-third of women currently aged 64 to 66 meet the criteria to exit cervical cancer screening.12 Age-related guidelines for discontinuing cervical cancer screening apply to only low-risk patients. As obstetrician-gynecologists, we are tasked with educating our patients and colleagues in other specialties about the importance of screening to prevent cancer.

Newsletter
Get the latest clinical updates, case studies, and expert commentary in obstetric and gynecologic care. Sign up now to stay informed.
In this episode of Pap Talk, Gloria Bachmann, MD, MSc, breaks down what it means to be a health care provider for incarcerated individuals, and explores the specific challenges women and their providers face during and after incarceration. Joined by sexual health expert Michael Krychman, MD, Bachmann also discusses trauma-informed care and how providers can get informed.
Listen
ADHD linked to higher risk of premenstrual dysphoric disorder
June 26th 2025Women with attention-deficit hyperactivity disorder are over 3 times more likely to experience premenstrual dysphoric disorder, especially when co-occurring with anxiety or depression, according to new research.
Read More
