View as a PDFDespite overall decreases in the national birth rate in the United States, the birth rate of cisgender women aged 35 to 45 years has increased over the past 3 decades.1 The choice to delay pregnancy is an intensely personal decision and has been linked to the pursuit of career advancement, lack of a suitable partner, or lack of readiness to have children.2 Oocyte cryopreservation is becoming an increasingly popular option, offering patients the opportunity to delay pregnancy while increasing the chance of conceiving at a later date.
Traditionally, oocyte cryopreservation has been reserved for select patients with medical indications, including those undergoing gonadotoxic therapies3 such as chemotherapy, patients with endometriosis or genetic predisposition to decreased fertility, and those pursuing fertility preservation in the setting of gender-affirming hormones and surgery.3 Since the 2013 decision by the American Society for Reproductive Medicine to lift its experimental label,4 there has been a 400% increase in demand for oocyte cryopreservation. Furthermore, the proportion of patients younger than 35 years electing to undergo cryopreservation has increased from 25% in 2012 to 35% in 2022.5,6 This increase is expected to continue as many companies begin to offer insurance coverage for this procedure as an employment recruitment strategy. Although the literature investigating outcomes related to pregnancies conceived via cryopreservation has yet to match this increase in demand, physicians must be prepared to counsel patients considering planned oocyte cryopreservation.
Counseling for age-related fertility decline
Age-related fertility decline typically begins in individuals aged 32 years,7 with more significant declines in individuals 37 years or older due to decreases in follicular number and oocyte quality secondary to age-related changes.8 Results from some studies have found that fertility level is highest in nulliparous patients aged 27 to 28 years and parous patients aged 29 to 30 years.9 Additionally, older age at time of conception is associated with increased rates of aneuploidy and fetal loss.10 Although planned oocyte cryopreservation cannot control for all risk factors associated with increased maternal age, preserving oocytes can reduce a patient’s risk of aneuploidy and improve the likelihood of a viable pregnancy. Pregnancies conceived spontaneously and via oocyte cryopreservation show comparable values in mean birth weight and rate of congenital abnormalities and developmental deficits.11 However, providers should communicate that there is a paucity of data about long-term outcomes in these children.
When considering whom to counsel on infertility, physicians should make all patients aware of age-related fertility decline. However, it is especially important to educate women in highly demanding professions who have been shown to experience higher rates of infertility and are older on average at the time of first childbirth.12
Expected success rates
Outcomes data regarding age-related pregnancy success rates after cryopreservation remain limited, because most women who have frozen their eggs have not yet returned to use them. Figure 1 shows a summary of expected success rates based on a leading cryopreservation counseling tool, but it should be noted that this tool is based on calculated projections of probability and not on actual outcome data.13 Retrieving and freezing eggs at a younger age correlates with higher likelihood of live birth when controlling for total oocytes frozen. Freezing eggs at a younger age also decreases the need for multiple cycles of oocyte stimulation and reduces the risk of aneuploidy associated with older oocytes.2 For women undergoing cryopreservation at an advanced age (mean 38 years), results from a small retrospective study found a 27% live birth rate per woman.14
Despite the benefits of early oocyte retrieval, providers should counsel patients on the need for longer storage and the resulting increased fees and about the possibility that patients may conceive without intervention, leading to cryopreserved eggs being unused.
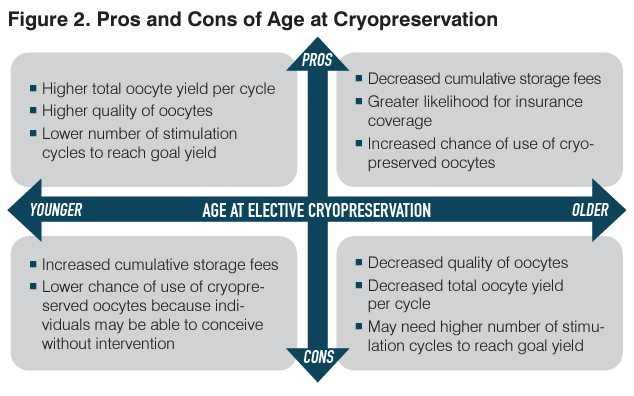
Figure 2 contains a summary of the pros and cons of undergoing planned oocyte cryopreservation at a younger vs older age.
Expected costs
The total cost of cryopreservation depends on the degree of insurance coverage. Patients should be counseled that there are multiple embedded costs in the process, including ovarian stimulation medications; lab and ultrasound monitoring; the oocyte retrieval procedure; anesthesia; oocyte cryopreservation; annual oocyte storage fee; fees associated with warming, intracytoplasmic sperm injection (ICSI)/IVF, and embryo culture; and the future embryo transfer procedure.15
Planned oocyte cryopreservation
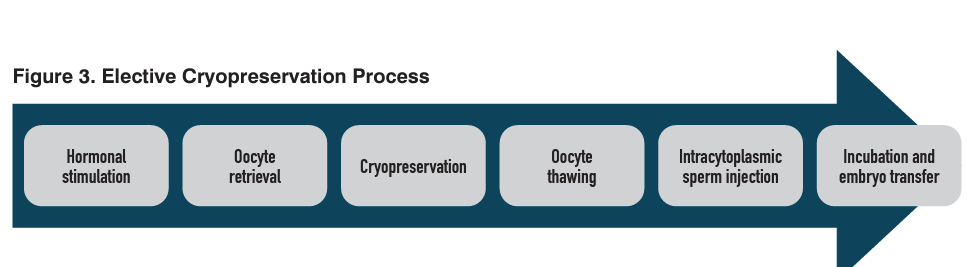
Your patient has decided to freeze their eggs. What should they know about the process before embarking on this journey? At the most involved level, the egg freezing process includes hormonal stimulation of the ovaries16; transvaginal oocyte retrieval; egg freezing and storage; and thawing of eggs, determination of viability, and use in ICSI/IVF to achieve pregnancy (Figure 3).
It is important to evaluate for other reproductive comorbidities such as polycystic ovarian syndrome, which may influence choice of stimulation regimen, and ascertain whether the patient has undergone prior ovarian stimulation cycles. Typical preprocedure testing may include follicle-stimulating hormone (FSH) and estradiol on cycle days 2 to 4; anti-Müllerian hormone; and height, weight, and body mass index. Additionally, baseline ultrasound imaging of the ovaries measures antral follicle count and ensures access to the ovaries for planned oocyte retrieval. Fertility laboratory tests, imaging, and a thorough fertility history prior to ovarian stimulation help inform which stimulation protocol is most appropriate.
An important message to convey to patients about cryopreservation is that the intent of a hormonal stimulation protocol is to induce and sustain the growth of multiple follicles leading to multiple oocytes. Importantly, exogenous ovarian stimulation does not deplete ovarian reserve; rather, more oocytes are sustained instead of undergoing natural atresia. During a normal cycle (without cryopreservation), the body similarly grows multiple follicles. However, only 1 oocyte fully develops, and the remainder of the follicles expire.
Controlled ovarian stimulation
A single cycle of ovarian stimulation usually takes approximately 10 days, with a goal of 10 to 20 oocytes per cycle.13 Higher yields are associated with younger age, but individuals 35 years or older can pursue multiple cycles of stimulation to account for lower quality and quantity of oocytes. However, for patients 40 years or older or with a diminished ovarian reserve, this strategy may not provide an adequate number of normal oocytes to be successful.
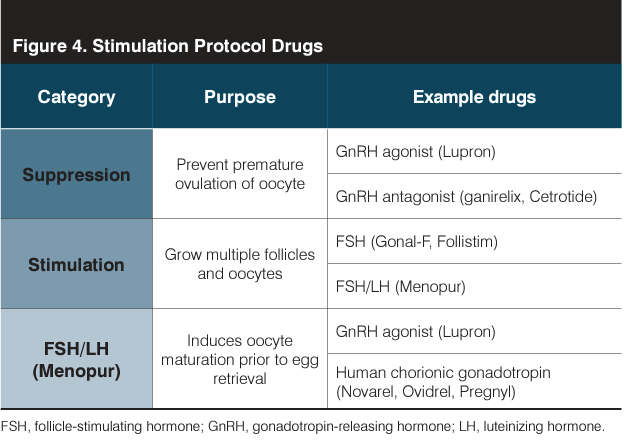
There are many stimulation protocols with varying drug regimens and doses. Regimens typically contain gonadotropic agents to stimulate follicle growth, an agent that stops eggs from ovulating prior to retrieval, and an agent that induces egg maturation. Sometimes oral contraception pills are used in advance of stimulation to regulate a patient’s cycle or suppress ovarian response for patients with hyperresponse. For those with elevated FSH levels (ie, diminished ovarian reserve), prestimulation estrogen priming can be used to normalize gonadotropin production via a negative feedback cycle. Figure 4 shows a summary of medications frequently used in ovarian stimulation.
Although doses of gonadotropin can vary among patients and protocols, enough must be used to ensure adequate egg harvest. However, gonadotropin doses that are too high are also associated with increased risk of ovarian hyperstimulation syndrome (OHSS)17 and increased cost.
Both long agonist and antagonist protocols have been shown to have similar efficacy when measured by live birth rates/cycle.18 With each cycle, a new cohort of follicles is stimulated. This means that even if a previous protocol resulted in low yield, the same drug regimen can still be successful in future cycles. During stimulation, patients receive frequent blood tests to monitor hormone levels and transvaginal ultrasounds to assess follicle count and growth. They also subcutaneously self-inject stimulation drugs daily.
Medication adverse effects
One of the primary concerns during the stimulation process is OHSS,18 a complication caused by exaggerated ovarian response to stimulation medications. It has been linked to use of human chorionic gonadotropin in stimulation protocols. Symptoms include abdominal pain, nausea/vomiting, ascites, localized or generalized peritonitis, dyspnea, hypotension/hypovolemia, hypercoagulability, electrolyte imbalances, and acute renal failure. The risk of moderate OHSS (ultrasonographic evidence of ascites) is 3% to 6%, whereas severe OHSS (moderate classificationplussevere abdominal pain and/or pleural effusion) occurs in 0.1% to 2% of all cycles. OHSS is typically self-limiting, but severe cases may require hospitalization, paracentesis, and/or anticoagulation. Additional adverse effects associated with gonadotropic medications (eg, Gonal-F, Follistim, Ovidrel, Menopur, and Luveris) include fatigue, headaches, weight gain, mood swings, nausea, breast tenderness, abdominal distension and pain, and ovarian cysts.19
Oocyte retrieval
Regardless of the stimulation protocol, mature oocytes are retrieved 34 to 36 hours after trigger shot administration—typically a human chorionic gonadotropin or gonadotropin-releasing hormone (GnRH) agonist—which induces resumption of oocyte meiosis. Oocyte retrieval is performed using a long needle under transvaginal ultrasound. The needle is guided transvaginally into each follicle, aspirating oocytes, granulosa cells, and follicular fluid. Intravenous sedation is used to minimize discomfort. Risks associated with retrieval, albeit small, are20:
- infection due to transfer of vaginal bacteria into abdominal cavity by needle(0.01%-0.6%),
- trauma to intra-abdominal organs with needle use(rare, described as case reports), and
- intra-abdominal bleeding as the procedural needle passes through a vascularized vaginal wall to obtain oocytes (0.02%-0.3%).
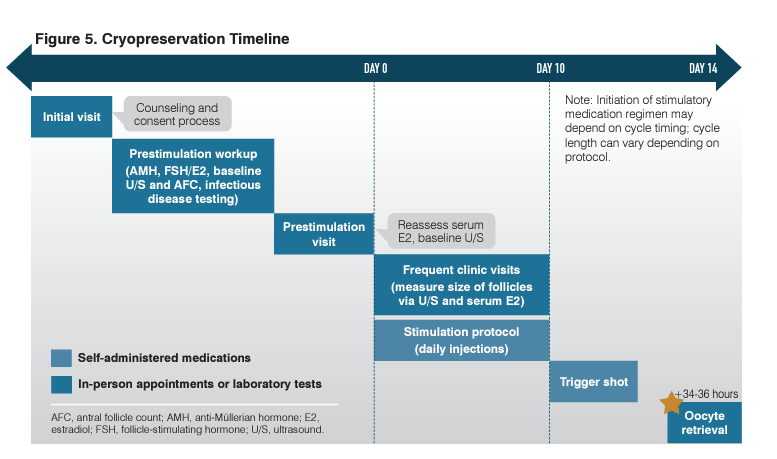
Providers should counsel patients on the risk that the procedure may fail to obtain any eggs or that the eggs may be abnormal or of poor quality, precluding a viable pregnancy. Patients may experience abdominal cramping immediately after retrieval and a heavier menstrual period, accompanied by more intense premenstrual syndrome–type symptoms, 10 to 14 days after the procedure, which is a result of hormonal stimulation leading to thickening of the uterine lining. Figure 5 provides a timeline demonstrating major milestones in the cryopreservation process.
Cryopreservation
Harvested mature eggs are frozen with a flash freezing method known as vitrification, which is now the preferred method of cryopreservation.21 The cumulus cells (ie, supporting cells) are removed from the eggs and the external shell known as the zona pellucida hardens with freezing.22 For these reasons, ICSI directly into the egg is recommended for fertilization. When comparing the use of fresh oocytes vs use of frozen oocytes that survive the thaw, clinical pregnancy rates have been shown to be equivalent.4,22
Thawing and fertilization
When patients are ready to attempt pregnancy, cryopreserved eggs are thawed. Estimated egg survival rates after thawing are 95% for women 35 years or younger and 85% for women 36 years or older.13 A single sperm is injected directly into the egg using a thin glass needle via ICSI. Embryos are incubated and ultimately transferred to the uterus on days 3 to 5 of development to achieve pregnancy.23 For patients desiring genetic testing, embryos can be biopsied and frozen on day 5 or 6. Genetically normal (euploid) embryos can later be thawed and transferred into the uterus.
Patients may also consider cryopreservation of embryos, especially patients with established partners or those who plan to use donor sperm. There are, however, important legal implications (varying by state) to consider when using a partner’s sperm. Because embryos contain genetic material from 2 individuals, there is a shared legal ownership and opportunity for either individual to prohibit their use in future pregnancies.
TAKEAWAYS
- Planned oocyte cryopreservation, or elective egg freezing, is becoming an increasingly popular procedure to combat age-related fertility decline as more individuals are choosing to delay pregnancy.
- Retrieving and freezing eggs at a younger age correlates with higher quality and quantity of oocytes per stimulation cycle, leading to greater likelihood of live birth when controlling for total oocytes frozen.
- Controlled ovarian stimulation with hormonal medications and oocyte retrieval, the same initial steps of in vitro fertilization (IVF), usually takes approximately 10 to 14 days to complete.
- When comparing the use of fresh vs frozen oocytes, clinical pregnancy rates are equivalent.
- Cryopreservation can be extremely costly and is only sometimes covered by health insurance, although coverage is increasing.
Limitations
Independent of the fertilization mechanism, pregnancies for women older than 35 years are at greater risk for preeclampsia, hypertension, and gestational diabetes and have a higher chance of requiring cesarean delivery.24 Although planned oocyte cryopreservation enables patients to increase the likelihood of achieving a live birth, it is crucial that clinicians counsel patients on the persistent risk factors associated with advanced maternal age pregnancies and the procedural risks, estimated costs, and factors influencing the likelihood of a successful pregnancy. Providers should also present alternatives to cryopreservation, such as adoption and use of donor oocytes, when exploring methods to grow families in the setting of potential future age-related infertility.
Although great strides in assisted reproductive technology have been made in recent decades, planned oocyte cryopreservation is not a foolproof insurance policy against infertility. Robust provider counseling that accounts for patient-specific values is needed to ensure patients make timely, informed decisions to ensure success.
References:
1. National Vital Statistics System (NVSS). Centers for Disease Control and Prevention. 2022. Accessed January 17, 2023. https://www.cdc.gov/nchs/hus/sources-definitions/nvss.htm
2. Goold I, Savulescu J. In favour of freezing eggs for non-medical reasons. Bioethics. 2009;23(1):47-58. doi:10.1111/j.1467-8519.2008.00679.x
3. Pai HD, Baid R, Palshetkar NP, Pai A, Pai RD, Palshetkar R. Oocyte cryopreservation - current scenario and future perspectives: a narrative review. J Hum Reprod Sci. 2021;14(4):340-349. doi:10.4103/jhrs.jhrs_173_21
4. Practice Committees of the American Society for Reproductive Medicine and the Society for Assisted Reproductive Technology. Mature oocyte cryopreservation: a guideline. Fertil Steril. 2013;99(1):37-43. doi:10.1016/j.fertnstert.2012.09.028
5. Gupta AH, Blum D. Hope, regret, uncertainty: 7 women on freezing their eggs. New York Times. December 23, 2022. Accessed March 14, 2023. https://www.nytimes.com/2022/12/23/well/family/egg-freezing-fertility.html
6. Final national summary report for 2019. Society for Assisted Reproductive Technology. 2019. Accessed February 2, 2023. https://www.sartcorsonline.com/rptCSR_PublicMultYear.aspx
7. van Noord-Zaadstra BM, Looman CW, Alsbach H, Habbema JD, te Velde ER, Karbaat J. Delaying childbearing: effect of age on fecundity and outcome of pregnancy. BMJ. 1991;302(6789):1361-1365. doi:10.1136/bmj.302.6789.1361
8. Faddy MJ, Gosden RG, Gougeon A, Richardson SJ, Nelson JF. Accelerated disappearance of ovarian follicles in mid-life: implications for forecasting menopause. Hum Reprod. 1992;7(10):1342-1346. doi:10.1093/oxfordjournals.humrep.a137570
9. Rothman KJ, Wise LA, Sørensen HT, Riis AH, Mikkelsen EM, Hatch EE. Volitional determinants and age-related decline in fecundability: a general population prospective cohort study in Denmark. Fertil Steril. 2013;99(7):1958-1964. doi:10.1016/j.fertnstert.2013.02.040
10. American College of Obstetricians and Gynecologists Committee on Gynecologic Practice and Practice Committee. Female age-related fertility decline: committee opinion no. 589. Fertil Steril. 2014;101(3):633-634. doi:10.1016/j.fertnstert.2013.12.032
11. Chian RC, Huang JYJ, Tan SL, et al. Obstetric and perinatal outcome in 200 infants conceived from vitrified oocytes. Reprod Biomed Online. 2008;16(5):608-610. doi:10.1016/s1472-6483(10)60471-3
12. Stentz NC, Griffith KA, Perkins E, Jones RD, Jagsi R. Fertility and childbearing among American female physicians. J Womens Health (Larchmt). 2016;25(10):1059-1065. doi:10.1089/jwh.2015.5638
13. Goldman RH, Racowsky C, Farland LV, Munné S, Ribustello L, Fox JH. Predicting the likelihood of live birth for elective oocyte cryopreservation: a counseling tool for physicians and patients. Hum Reprod. 2017;32(4):853-859. doi:10.1093/humrep/dex008
14. Tsafrir A, Ben-Ami I, Eldar-Geva T, et al. Clinical outcome of planned oocyte cryopreservation at advanced age. J Assist Reprod Genet. 2022;39(11):2625-2633. doi:10.1007/s10815-022-02633-7
15. Mesen TB, Mersereau JE, Kane JB, Steiner AZ. Optimal timing for elective egg freezing. Fertil Steril. 2015;103(6):1551-6.e64. doi:10.1016/j.fertnstert.2015.03.002
16. ART: step-by-step guide. Society for Assisted Reproductive Technology. 2023. Accessed February 2, 2023. https://www.sart.org/patients/a-patients-guide-to-assisted-reproductive-technology/general-information/art-step-by-step-guide
17. Delvigne A, Rozenberg S. Epidemiology and prevention of ovarian hyperstimulation syndrome (OHSS): a review. Hum Reprod Update. 2002;8(6):559-577. doi:10.1093/humupd/8.6.559
18. Kadoura S, Alhalabi M, Nattouf AH. Conventional GnRH antagonist protocols versus long GnRH agonist protocol in IVF/ICSI cycles of polycystic ovary syndrome women: a systematic review and meta-analysis. Sci Rep. 2022;12(1):4456. doi:10.1038/s41598-022-08400-z
19. Gonadotropin stimulation. Society for Assisted Reproductive Technology. 2023. Accessed January 14, 2023. https://www.sart.org/patients/a-patients-guide-to-assisted-reproductive-technology/stimulation/gonadotropin-stimulation/
20. Bodri D, Guillén JJ, Polo A, Trullenque M, Esteve C, Coll O. Complications related to ovarian stimulation and oocyte retrieval in 4052 oocyte donor cycles. Reprod Biomed Online. 2008;17(2):237-243. doi:10.1016/s1472-6483(10)60200-3
21. Poli M, Capalbo A. Oocyte cryopreservation at a young age provides an effective strategy for expanding fertile lifespan. Front Reprod Health. 2021;3:704283. doi:10.3389/frph.2021.704283
22. Cobo A, Meseguer M, Remohí J, Pellicer A. Use of cryo-banked oocytes in an ovum donation programme: a prospective, randomized, controlled, clinical trial. Hum Reprod. 2010;25(9):2239-2246. doi:10.1093/humrep/deq146
23. Van Voorhis BJ. Clinical practice: in vitro fertilization. N Engl J Med. 2007;356(4):379-386. doi:10.1056/NEJMcp065743
24. Pregnancy at age 35 years or older: ACOG obstetric care consensus no. 11. Obstet Gynecol. 2022;140(2):348-366. doi:10.1097/AOG.0000000000004873